 Anatomic studies have reported common safe zones within 2.7 cm of the sternoclavicular joint and 1.9 cm of the acromioclavicular joints thus leaving the nerve vulnerable to injury during the approach to the most common fracture pattern, i.e., involving the middle third diaphysis. It may have two or three branches and their courses have notable variability, with one case report of a transosseous path, making its identification difficult. It pierces through the platysma crossing the clavicle 97% of the time, most commonly over the lateral two thirds, to provide sensation to the anteromedial shoulder and upper chest wall. The supraclavicular nerve is at risk of injury during clavicle fixation. Post-operative sensory disturbances have been variably linked to patient experience in other orthopaedic procedures. 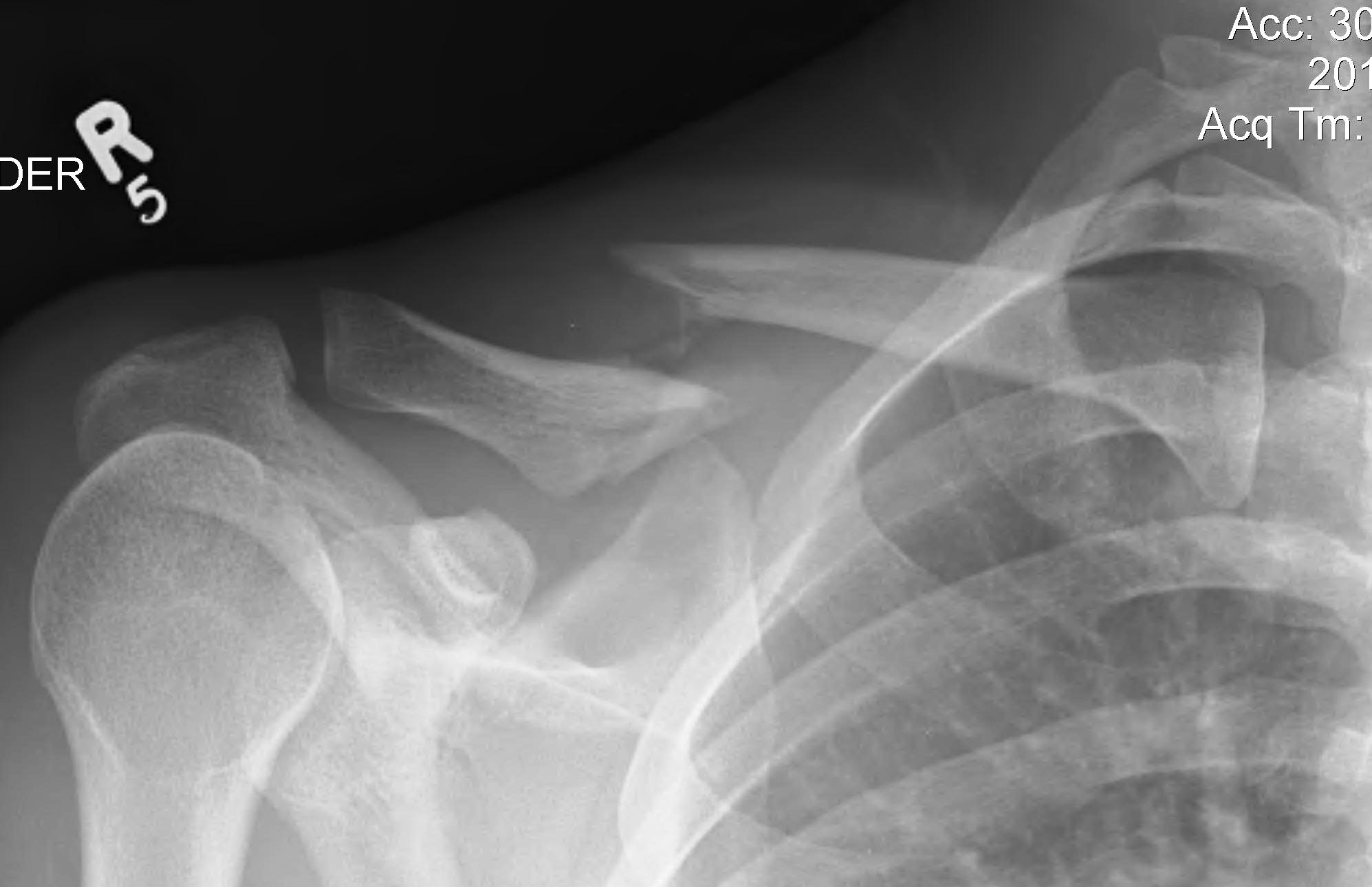
The lack of clear operative benefits and well-defined indications necessitates improved understanding of the patient experience in order to deliver optimal patient-centered care. Controversy persists as cost-effectiveness of surgical intervention remains unclear and recent meta-analyses failed to demonstrate clinically significant benefits in patient function. Consequently, a trend towards operative management has emerged with good overall outcomes. Traditionally, these fractures were treated non-operatively, but studies have since demonstrated improvement in union rates, less fracture deformity, and earlier return to function, following surgical stabilization. They most often occur in young males and in the middle third of the bone. Patients should always be advised of the risk of persistent sensory alterations around the surgical site to increase the likelihood of their satisfaction post-operatively.įractures of the clavicle are common, accounting for 2.6–4% of all fractures and 44% of fractures involving the shoulder girdle. While most patients improve, some symptoms persist in the majority of patients without significant negative effects on satisfaction. Post-operative sensory disturbance is common. Patients who experienced burning were less satisfied overall with the outcome of their surgery whereas those who were informed of the risk of sensory changes pre-operatively were more satisfied overall. Numbness was the most common symptom (64%) and complete resolution occurred in 32% of patients over an average of 19 months. 
Ninety percent of patients experienced sensory changes post-operatively. Correlations between demographic factors and outcomes, as well as subgroup analyses were completed to identify factors impacting patient satisfaction. MethodsĮighty-six patients were identified retrospectively and completed a patient experience survey assessing sensory symptoms, perceived post-operative function, and satisfaction. This study aims to determine the prevalence, extent, and recovery of sensory changes associated with supraclavicular nerve injury after open reduction and plate internal fixation of middle or lateral clavicle shaft fractures. In the context of explaining the risks and benefits of surgery, understanding the impact of incisional numbness as it relates to the patient experience is key to shared decision making. Operative management of clavicle fractures is increasingly common. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
